
- Cody Wymore, teenage son of Sergeant Tim Wymore, on the deck of the family home in St. Charles, Missouri. Cody fears that his father, whom he believes was poisoned by working at the burn pit on the Balad Airbase in Iraq, will not live to see him reach adulthood. (nina berman)

- Tim Wymore, hoping to document the source of his health problems, snapped this picture of the Balad burn pit before leaving Iraq.
That funk.
No one had to explain to Tim Wymore or LeRoy Torres or any of the other troops and contractors why they couldn’t breathe.
The burn pit on Balad Airbase in Iraq had a life of its own. Black smoke and orange flames shot heavenward twenty-four seven. Big as five football fields. Ten acres easy. Lit up the whole night sky. When the seasons changed and the winds died and the air didn’t move, the smoke just hung, a stagnant mass over the whole base.
Do the math, Tim tells me. Thirty thousand troops, eight bottles of water a day. Thirty thousand times eight, that’s the bare minimum of how much plastic was burned daily. Thirty thousand times three Styrofoam plates a day in the chow hall. Most guys got second and third helpings. Every day, every meal. That’s a lot of trash, but that ain’t half of it, he says. Add in the arms and legs of amputees, the blood of the dead and wounded, needles, IV bags, coffee cans, plastic tubing. Loads of old computers.
All of it up in smoke for everyone to breathe, LeRoy says. Pain twists his stomach. A doctor told him to change his diet. This isn’t about what I eat, he said.
All these months later, Tim and LeRoy still taste it, like burning copper pennies in their mouths. Brush their teeth but it doesn’t help. That was the first clue. If the taste stayed this long, what else remained, filtered down, spreading through their bodies?
I was in the waiting room of my doctor’s office, cruising the internet on my laptop, when I read some news stories about burn pits. A growing number of military medical professionals blamed the pits for causing a wave of respiratory and other illnesses among troops returning from Iraq and Afghanistan. Found on almost all US bases in the war zones, these open-air trash fires disperse dioxin, carbon monoxide, and other chemicals over the living and working areas of coalition forces and local civilians.
According to the Department of Defense, US military operations in Afghanistan and Iraq generate about ten pounds of solid waste per soldier each day. The military has relied on open pit burning to dispose of this waste since the start of the wars mainly because of its expedience. In August 2010, United States Central Command estimated there were 251 burn pits in Afghanistan and 22 in Iraq. The Balad burn pit, one of the largest, was extinguished in 2009. It had burned almost continuously since US troops first arrived in 2003.
Last year, a lawsuit was filed alleging that Kellogg Brown and Root (KBR), and its former parent company Halliburton, one of the US military’s largest contractors, had endangered the health and safety of American soldiers in Iraq and Afghanistan by exposing them to huge quantities of toxic dust, fumes, and other air pollutants. KBR allegedly burned unsorted waste with such disregard that thick, noxious smoke (sometimes colored blue or green by burning chemicals—the kinds of chemicals that firefighters back in the States wear masks and oxygen tanks to protect against) drifted and hung over US bases and nearby towns for days, or even weeks, at a stretch.
The nurse called my name. I had returned from a reporting trip to Afghanistan two months earlier and was experiencing a weird pressure on my chest, a kind of weight that made me feel slightly out of breath. I was also having severe coughing fits that erupted out of nowhere, lasted minutes, and left me gasping for air as if I had been choking.
I assumed it was allergies, or maybe the resumption of the asthma I had as kid. I had also recently gotten a new cat; maybe I was allergic. I have mild shortness of breath, I told my doctor using the stilted language I associated with doctors so that I would sound knowledgeable. He checked my blood pressure, listened to my chest. He gave me a breathing test to determine lung strength. I took a deep breath and exhaled as hard and as long as I could three times into a tube. My head swam dizzily with the effort. The doctor looked at the results.
This isn’t mild shortness of breath, kiddo, he said. When was your last chest x-ray?
The x-ray showed enlarged lymph nodes in my lungs. A CT Scan confirmed the x-rays. The doctor said he did not believe it was cancerous. He assumed I developed a lung infection in Afghanistan which led to an irritation of the lymph nodes. Don’t panic, he said, but you’ll have to come see me every four months.
I left panicked.
I wondered if I had been exposed to something during my 2003 embed with the Army. That was a while ago, but I have traveled to Afghanistan every year since then, and have spent a fair amount of time on military bases. I wondered what I might have inhaled. I wanted to know more. Through the office of Disabled American Veterans, I was given the names of Tim Wymore and LeRoy Torres, two sick Iraq war veterans who blamed burn pits for their ills. I wanted to meet them, learn about their condition and, selfishly I suppose, see if I could figure out what was happening to me.
Tim Wymore and his wife Shanna live in a compact two-story house on a narrow street in St. Charles, Missouri. On this January day snow conceals parked cars and smoke drowsily rises from chimneys. I walk up the driveway, past two large trucks and into the garage where a door leads to the kitchen. A fire blazes in the living room fireplace keeping the temperature close to eighty. Among other problems, Tim suffers from constant chills. Despite the heat, he wears a sweatshirt and sweatpants.
At first, I see nothing about Tim to suggest illness. He lies on a couch, a stocky guy who offers a gentle handshake. Then I notice the plastic tubes in his nose and the oxygen machine at the end of the couch. Tim lets go of my hand, rolls on his side and shuts off the oxygen. The sudden absence of its gurgling makes the silence palpable. Tim removes the tubes from his nose and sits up. Tim looks blankly at their large flat screen TV. News. Major winter storm coming. He flips channels. Price Is Right. He sinks back in the sofa, volume off.
He tries not to use oxygen too much, he tells me, but Shanna insists, especially when she sees his face grow pale and dark rings begin forming below his eyes.
I feel a frickin’ headache coming on, he says.
Doctors say the headaches are a result of too much oxygen. Another meaningless diagnosis as far as Tim is concerned. Doctors have diagnosed him with post-traumatic stress disorder but offer no answers about his physical ailments. Tim takes twenty-six medications including morphine. He has lesions on his brain and eye. All his muscles ache. He can barely stand, let alone walk. He suffers from blood disorders, damage to his esophagus and lungs, and abdominal problems that finally forced the removal of most of his colon. He can’t put his clothes on without help. Can’t even put socks on. Just a simple walk down the hall and he loses his breath. If he tries walking too much his heart rate soars.
Tim joined the Air Force National Guard in 1998 after three years serving active duty. All of his uncles had been in the Air Force; one did two tours in Vietnam. In 2004, Tim was called up for duty with the 131st Fighter Wing based at Lambert-St. Louis International Airport. To his surprise, he was deployed to Iraq—one of only five members of his unit sent overseas. He didn’t tell Shanna right away. When he did, she started crying. He worried about her and their three boys. He didn’t think he was coming back. He arrived in Kuwait and from there flew to Balad.
As a technical sergeant, Tim drove a tractor trailer, moving goods around the base, including several trips a week driving loads of garbage into the burn pit. Once, he took twenty-five loads of unserviceable tents left from the Persian Gulf war into the pit. No telling what chemicals had been sprayed on them. DEET for sure, god knows what else. The Army even dumped Humvees into the pit and then ordered new ones. Poured jet fuel on the entire mess and let it rip.
Once it started, the pit stayed burning. There was always something to feed into it. Every time Tim hauled a load over he remained inside the truck cabin, gagging behind the wheel, surrounded by soot and dense smoke. Clouds so thick he couldn’t see, heat so intense it was like he was on fire. He had asked for a mask but was told masks weren’t necessary.
Iraqis often dug in the pit for scrap metal. They tried to load shit up, but they had so much they couldn’t lift it. Tim tells me they were getting sick too. Who took care of them? He didn’t know. Beyond the base’s barbed wire fences, a creek ran off a canal and the ground was green with grass. Inside the base, the Army planted rows of palm trees but not one lived. Nothing grew.
Tim shifts his weight on the couch, waits for Shanna to get off the phone so he can use the bathroom. She is talking with Rosie Torres, LeRoy’s wife. They met through a Facebook group, where families of sick veterans exposed to burn pits offer one another support and information, including the details of their experiences with doctors, the US Department of Veterans Affairs, and disability applications.
As we wait for Shanna, I riffle through a file box near the fireplace, filled with Tim’s medical records, and dozens of hospital wristbands.
I pull out a sheaf of papers with the date April 26, 2010. Sent to all regional Veterans Affairs offices by the VA and headed: Environmental Hazards in Iraq, Afghanistan, and Other Military Installations.
I flip through it.
Polycyclic Aromatic Hydrocarbons are a group of over 100 different chemicals formed during the incomplete burning of coal, oil, gas and garbage, or other organic substances. Some of the PAHs that were tested for and detected are listed below. These results are from DOD testing at Balad from January through April, 2007.
A dozen PAH compounds are known or probable human carcinogens. Even the non-carcinogenic compounds have been linked to asthma and other respiratory problems. Symptoms include cough, wheezing, and bronchitis.

- Shanna Wymore puts Tim to bed with an oxygen mask to help him breathe while sleeping. She says she used to struggle to keep up with him. (nina berman)
More chemicals are listed under the category: Volatile Organic Compounds Released as Gases from Certain Solids or Liquids. Still more are listed under: Toxic Organic Halogenated Dioxins and Furans. The list of chemicals resembles an algebraic concoction: 1,2,3,4,6,7,8 HPCDD, 1,2,3,4,6,7,8 HPCDF1,2,3,4,7,8,9 HPCDF, 1,2,3,4,7,8 HXCDD—and on and on.
Is this what Tim pulled into his lungs? Is this why I’m coughing and always out of breath?
Shanna hangs up the phone and comes to wrap her arms around Tim and help him into a small motorized cart parked by the couch. Down the hall, she helps him out of the cart and into the bathroom and shuts the door.
Two days later, I drive to the Torres home in Robstown, Texas, near Corpus Christi. Barren cotton fields stretch into the horizon beside rutted county roads. A stray bulldog has taken residence on their front stoop. The dog stays outside but LeRoy wraps a blanket around it at night.
Before I left Missouri, Shanna told me that LeRoy was nervous about meeting me. He does not look sick any more than Tim does when he is not on oxygen, she explained. And indeed, the muscular thirty-eight-year-old man who greets me at the door in jeans and a wool shirt does not appear ill. But then, I listen to how softly he speaks, a cross between a whisper and breathlessness. On the cluttered kitchen counter, near a coffee machine, I notice a stack of nine medications. LeRoy explains he no longer takes any of them. Old meds his doctors prescribed but now agree are ineffective for whatever ails him. I look at one; an Asmanex Twisthaler. My doctor gave me that one, too.
After offering me coffee and asking about my drive, LeRoy excuses himself. He needs to take his daily twenty- to thirty-minute nap, a ritual he has come to reluctantly accept. By mid afternoon of most days, and for reasons he does not understand, he feels his energy drain out of him, and his body become wracked with chills.
LeRoy climbs into bed, covers himself.
I ask him, What goes through your mind at these times?
How long will I be like this? Will I be better? Will I be normal again, the way I used to be?
He tells me about a dream. He was parked outside his mother’s house in his truck. He got out and started coughing. He couldn’t find his inhaler. He reached for the front door and woke. Rosie has dreams too, he says. She dreamed of a soldier in a coffin wearing his military uniform. She looked at his face. It was LeRoy. He had to calm her when she told him. He sighs, adjusts his blanket.
I glance around the room, some rumpled clothes scattered across the floor. LeRoy’s tan state trooper uniform still hangs on his closet door. He left it there when he went to Iraq, a reminder to Rosie and himself that he would come back. A reminder of his passion for the job he had aspired to since he was a kid. He wants to believe he will wear it again.
But, in October, the Department of Public Safety removed his squad car, his black and white from his home. He had been on official leave since September because of his persistent cough. You’re going to get everybody sick, his supervisor had told him. For security reasons alone his vehicle could not remain sitting unused in his driveway with guns in it. Best thing to do was take it back to the station, LeRoy says. But watching it drive off hurt worse than all the pains afflicting his body, worse than this exhaustion that forces him into his bed on a Thursday afternoon.
A member of the Army reserve, LeRoy flew to Kuwait in 2007 with the 402nd Army Field Support Brigade out of Rock Island, Illinois, just a week before Thanksgiving. Oh goodness, it was hot and dusty, he recalls. Balad, where his unit was stationed, was even dirtier. The 402nd was hammered quite a bit by incoming fire during the first six months. The mortars came in so frequently that the guys starting calling the area where they lived Mortarville.
The stink of Balad’s burn pit struck him the minute he walked off the plane. Sometimes sandstorms dispersed the black smoke but it always returned. Grime all over vehicles. He would wipe chalky charcoal-like dust off his air conditioning unit. He tried not to go near the pit but the smoke hovered over Balad thick as a winter blanket. He couldn’t avoid it.
Within a week of returning home in 2008, he developed a cough and had difficulty breathing. A doctor told him he had an upper respiratory infection. Maybe bronchitis. Your lungs are just trying to clear themselves after being in Iraq, the doctor said. But LeRoy could not get rid of his cough. He’d feel better and then get sick again. He was given an inhaler, but the cough remained.
Last spring, exhaustion overwhelmed him. He took breaks at work. Parked at the side of a road in his squad car, he fought against falling asleep. A simple traffic stop wore him out. He could no longer run his daily mile.
In October 2010, LeRoy and Rosie flew to the VA’s War Related Injury and Illness Center, in Washington DC. There, doctors found lesions and a parasitic infection in his spleen. They also diagnosed sleep apnea. But despite his coughing and wheezing, doctors found nothing wrong with his lungs.
The following month, at Vanderbilt University Medical Center in Memphis, doctors performed a biopsy on his lungs, and LeRoy was diagnosed by Dr. Robert F. Miller, his physician, with constrictive bronchitis, a condition associated with toxic inhalation. LeRoy’s airways were permanently damaged.
Is it progressive? LeRoy asked. Dr. Miller did not think so.
LeRoy had more questions that he kept to himself. How long will I live? How long will I get to see my kids?
He spoke to his supervisor at the Department of Public Safety about his diagnosis. The supervisor would try to find LeRoy another position within the department. LeRoy understood. He knew he could not remain on the street and risk suffering a coughing fit while chasing a suspect. But understanding did not make the decision less difficult to accept.
There goes my job, he told Rosie.
Sometimes, when he feels discouraged, LeRoy calls Tim. At these times, Tim does not reveal his own despair. That he has reached a point of just-screw-it. I’ll live the rest of my life the way it is now. He resents telling each new doctor his story over and over again. Why can’t you pee? I don’t know. You’re the doctor.
You know you’re going to get through this, Tim will tell LeRoy. It’s not our fault. They want us to give up. We can’t give up. We have to stick together. Call me any time.
I appreciate that, LeRoy says.
I’ve been there. There have been days I’ve cried my eyes out. Doesn’t make me less of a man. Or you. We’ve been through hell.
Yes, LeRoy says.
Literally hell, Tim says.
While LeRoy takes his nap, I call Doctor Miller at Vanderbilt. He has become the de facto expert on illnesses related to burn pits. His research began after he treated a female veteran who suffered severe shortness of breath after being stationed at Balad. In the three years since then, Miller has diagnosed more than fifty soldiers with constrictive bronchitis; all were exposed to burn pits. And now, with his reputation spreading, the numbers are climbing fast. He sees two to three new cases a month. On the phone, Doctor Miller is helpful but speaks with the detachment of his profession.
Early in the war, he explains, it was impossible to avoid burning human waste and garbage because there were no incinerators. That’s something we don’t even allow in this country, but that’s what the army does. It burns things.
Smoke contains particulates, tiny solid particles suspended in the air—dust and sand for instance. When we inhale, we don’t just breathe in air; we also get anything suspended in it. The particles can stick to the sides of the airway or travel deeper into the lungs. The worse the particulates, the worse the illness. And the farther the particulates travel into the respiratory system, the worse the effect. But it’s more than that, Miller concludes. Smaller, lighter particles, like those in many toxins, can remain in the air longer and can travel many hundreds of miles. People stationed at Balad may have the worst of it, but anyone who has spent significant time in Iraq or Afghanistan may be at risk.
I realize as he says this that I might very well have inhaled something while I was in Afghanistan, especially in 2007 when I experienced daily, uncontrollable coughing fits. That summer in Kabul there was plenty of dust blowing through the streets. Where it had originated from and what it carried I have no idea.
Dr. Miller’s findings do not sit well with the military. As of August of last year, all of his veteran patients have been referred to Brook Army Medical Center in San Antonio. The center does not have the facilities to perform the lung biopsies necessary for a diagnosis of constrictive bronchitis. Without such a diagnosis, the veteran won’t receive a disability rating needed to determine a disability payment.
The general consensus is that defining all of this will cost a lot of money, Miller tells me. The Department of Defense would much rather have the VA pick up the tab. If you get a disability rating while still active in army, the army has to pay. A low rating in the army, but a high post deployment rating, means the VA pays. It’s partially a matter of who can limit financial exposure.
Miller thinks eventually veterans will be compensated, but it may take years—and legal action.
I think this will end up like Agent Orange, he says.
Shanna has reached a similar conclusion when I see her again.
It will just be like Agent Orange, she tells me, smoking a cigarette in her garage. Twenty-five years down the road they’ll admit there was a problem.
Of course, by then it will be too late.
Shanna had no idea what a burn pit was when Tim was in Iraq. Tim sent her pictures but she thought the black smoke was from an explosion.
She exhales a long cloudy breath that vanishes over Tim’s Harley. He’ll ride it again some day. That’s his goal.

- Tim Wymore’s headaches are worsening, likely the result of lesions on his brain and one of his eyes. His wife Shanna had to quit her job to care for him full time. (nina berman)
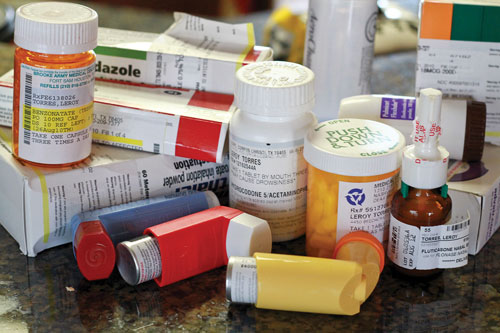
- LeRoy Torres’s kitchen counter is piled with medications, but doctors have not found an effective treatment.
Shanna feels trapped. Just the other day, Tim was seen for rheumatoid arthritis for the third time by a third different rheumatoid arthritis doctor. Another doctor told Tim his spine was deteriorating. Old age, the doctor said. He’s forty-four, Shanna reminded the doctor. Let me tell you something, I’m the same age. My spinal cord ain’t deteriorating.
Now they want him to stay overnight at the VA for sleep apnea. But he did that eight months ago, she says, her voice rising. He stopped breathing ninety times. So this time it might be one hundred ten times, so? What will they tell her? Turn up his breathing machine again?
Why, she wants to know, isn’t anyone worried about what’s happening to his organs, the brain lesions? Today is one of those days she feels on fire. Like Tim says: no more appointments; no more seeing someone just to see someone.
Shanna taps her foot, tears in her eyes, and thinks that the deer head on the garage wall behind her needs to be raised. Everyone bumps into it walking around her truck. An idle thought. Her mind races, unfocused, scared.
She woke up at four this morning, slipped on a t-shirt and a pair of sweats and pinned her blonde hair in a pile on top of her head. By eight she had already vacuumed the house. Only had two, three hours of sleep. She rarely leaves the house. What else can she be doing for Tim? And they wonder, she says shaking her head, why people go crazy.
Look at her datebook. Every square filled with a doctor’s appointment for Tim. At one time, Shanna sold industrial tools and supplies. She was a real estate agent. Tim was a machinist. They had hoped to retire by fifty.
Not now. Tim hasn’t worked since December 2009. Shanna quit to care for him. He can’t be left alone. Even if he could, would drive him to his appointments?
Shanna was unaware Tim had been sick in Iraq. He never told her. When he came home, he kept having stomachaches and headaches. He passed out in bed, blacked out at work. Here she had been thinking their life would resume as before.
As Shanna smokes, Tim looks through some papers he printed off the internet about a Dallas hospital that treated 9/11 first responders. He wants to go there. He reads that the doctors can laser toxins right out of your body. Use heat and sauna type stuff. All natural. But he has to be referred by a doctor. The VA doesn’t want to pay for it. Tim thinks they don’t like natural treatments. His social worker presented the idea to them. Not FDA approved, he was told. A Missouri state representative said he would get Tim to Dallas. But then there were the November elections, then Christmas, then New Year’s, then all the time it takes for people to catch up after the holidays. More time lost.
One night, Rosie Torres hugged LeRoy and thought: this is not my husband. When they married, she could rest her head on his chest, her black hair splayed about her shoulders, shrink into his bulk and feel safe. He weighed about 238 pounds then, most of it muscle.
She doesn’t feel safe anymore.
I don’t know where he is, she says.
LeRoy’s weight has dropped to 218 pounds. At night, Rosie listens to him breath, hears crackling noises in his throat. What is that sound?
She recalls a moment after he returned from Iraq. They were home and LeRoy started choking. Not from anything he had eaten or drunk. Just out of the blue. He ran to the bathroom gasping for air. Rosie screamed: What’s wrong? LeRoy stared at her with this please-help-me look—but she couldn’t. She yelled for her eldest son, Chris, who knows CPR. Dad, Chris said, look at me. Just breathe in and out, in and out.
Dad all right? Kenny, their second son, asks her now while Rosie prepares dinner.
He’s tired. Stomach bothering him again.
Chris and their daughter Merissa stay with Rosie’s sister in San Antonio. Rosie and LeRoy spend so much time at doctor’s appointments that someone had to watch them. When necessary, Kenny stays with family or friends in Robs-town. He immerses himself in sports. He doesn’t like to come home and see his father in bed.
Chris and Merissa talk to their parents every day. The children say, mom we just want to be home. As soon as they wrap up all these medical problems, they’ll get together again as a family, Rosie tells them. To herself she admits she doesn’t know when that will be.
One time she told LeRoy, I don’t have support here. I need to go to San Antonio where I have parents, my brother, a sister. Would he come with her?
He was born and raised in Robstown, he reminded her. His mother lives here.
Bring her, she said.
She won’t leave.
LeRoy.
If you need to go, go, LeRoy said. But I have to stay here.
Rosie stayed too. When one is weak, she tells me, the other must be strong.
Tim and LeRoy let me go with them to their doctor’s appointments.
On a Tuesday, Tim and Shanna visit Jefferson Barracks Division of the St. Louis VA Medical Center where Tim has his bladder examined to determine why he is having trouble urinating.
Four days later, LeRoy sees a doctor at Baylor College of Medicine in Houston about his stomach pains. The doctor prescribes an antidepressant that he says is effective in treating pain.
You have pain without evidence of a physical cause, the doctor tells LeRoy. We could do an x-ray for vascular abnormality. CT scan with oral contrast. But these are expensive tests.
He pauses. I don’t know, he concludes. There just are a lot things we don’t know.
Tim’s appointment proves equally disappointing. After an examination, a nurse tells Shanna that Tim has a possible blockage in his bladder. He needs further tests.
Is it cancer? Shanna asks.
If there is a blockage they’ll do a biopsy, the nurse says.
A lot of burn pit patients have bladder problems.
I don’t know about that, the nurse says.
A page from a June 2010 report by the US Army Public Health command, advising its personnel on how to deal with people who were complaining about exposure to health risks, including burn pits:
4.4.3 Communicating with other stake-holders (e.g. military family members, local nationals)
• Anticipate the most difficult questions/allegations and develop key points to reference in all potential responses
– What are you going to do about the mold growing on my ceiling since it just started after Camp X was put down the road?
– I have lung cancer and I know it’s from your burn pits!
– What was my husband exposed to at Camp X that could have caused his current health problems?
– What kind of long-term health effects can I expect because I’ve been living near Camp X for so long?
– Why didn’t you all tell us about this exposure before?
• Develop key messages/points that support the OEH assessment process and/or results, but that also balance interests/concerns of the layperson.
• Practice responding to difficult questions to increase your skill and confidence level (see Communicating with Soldiers section above)
While I was in St. Charles, Shanna put me in touch with Russell Keith, a contractor who served in Balad. At one time there were 120,000 troops on the ground in Iraq and about 135,000 contractors. Eight thousand contractors sometimes worked in Balad alone.
Russell had been a paramedic for years when he flew to Balad, as a contractor for KBR. Just after he landed at the base, a mortar exploded at the far end of the runway. Sixteen people refused to leave the plane. Their trip to Iraq from Kuwait lasted less than one hour.
Burn pits were not even acknowledged back then, Russell said. Got so bad flights into Balad were delayed because of a lack of visibility. Russell did healthcare orientation two times a week for new arrivals. Watch out for scorpions, watch out for snakes. Watch out for houseflies. There are bugs here you haven’t seen before. You’ll go through Benadryl like crazy. Russell showed photos of the burn pits with the caption: Okay, folks, you realize there’s no EPA over here.
Everybody chuckled. You all laugh, Russell told them, but in twenty years we might be in a class action lawsuit. More laughter. He distributed cough meds and decongestants like M&Ms. Some couldn’t breathe without them.
Few people could. You were in Balad for no more than ten minutes, Russell says, and you smelled and tasted the burn pit. You’d go, God, what are they burning? Absolutely stopped you cold. It was like somebody burning a refrigerator with food in it. Man, some nasty air over there.
One day in March 2007, the Air Force called an all-hands meeting and distributed particulate masks to wear outside. No one would explain why, what had changed. Russell considered the mask a knee-jerk reaction—someone had suddenly become worried about something. Russell figured it wasn’t a good sign. If the military had wanted to install air-scrubbing incinerators, it could have, he says.
Russell was in the clinic one afternoon when the pinkie on his left hand stiffened.
I’m just getting old, he thought. His left hand was cold. Freezing. He went home on R and R and saw a neurologist. In April 2009, Russell was diagnosed with Parkinson’s disease.
There was no history of it in his family.
His doctor asked him: Have you been exposed to pesticides?
Exposed? Russell said, I’ve breathed them.
Russell gives me the name of Anthony Szema, head of the allergy diagnostic unit at Stony Brook University hospital, who, like Doctor Miller at Vanderbilt, has also studied the health consequences of burn pits.
Doctor Szema tells me during a telephone interview that he still remembers when he walked into his waiting room in 2004 and instead of seeing ailing 80-something World War Two vets, he saw eighteen-year-old men and women back from Iraq with asthma and allergies. One kid had been an all-state football player. Joined the military, came back with asthma.
At the time, he had not known about burn pits. He thought the vets were sick from inhaling sand. Sand storms are so frequent in Iraq, the Iraqis name them, like creatures, or spirits, he tells me. With so many convoys and construction projects, the movement of war stirred up even more sand, adding to the particulates whipped up by the sandstorms.
On top of this were all the incendiary things. IED explosions, oil fires. Mortar rounds that contained depleted uranium. Soldiers were breathing all that, too.
Finally, there is the dust, different from the sand. Sharp, porous stuff. Particulates like metals or chemicals can cling to the coarse edges of dust particles, forming tiny globs of floating matter. Millions of microscopic particles of dust can carry lots of stuff, and all of it can lodge in a person’s lungs.
What is inside this dust blowing all over Iraq? Szema asks, rhetorically. No one really knows. The general public, Szema continues, is not aware of the implications of these exposures. No one has studied what happens when thousands of carcinogens burn at once in a pit, become airborne, and are inhaled by people around the clock for extended periods.
Everybody over there has been exposed, Szema says before we hang up. Iraq, Afghanistan, I guarantee they have been exposed.
One evening, Shanna talks with Aubrey Tapley, a thirty-one-year old Army reservist who was also stationed at Balad Air Base. The women sit at the kitchen table while Tim Wymore sleeps on the couch. Aubrey has been experiencing symptoms similar to Tim’s. Shanna tries to help her think about what to do next.
What’s your rating? Shanna asks.
I have ratings for headaches, Aubrey says. Fifty percent. I had one for three weeks. Pulling my hair out at work it hurt so much.
So are Tim’s. Now they are so bad his eyes roll back in his head. PTSD?
I’m rated for that.
Chronic pain on your rating?
No.
Shoot for that one.
Why was she so sick, Aubrey asked herself when she left Iraq in 2004. For five years she thought she was nuts. Then she met Shanna through the burn pit page on Facebook, and she saw for the first time that other vets were having similar problems. Like exhaustion. Sleeping until mid morning then taking a nap at noon. Up at four or five in the afternoon. Back in bed by nine. Like an out-of-body experience. She wanted to move, but her body defied her.
Spit same thing Tim does? Shanna asks.
Yes, it comes out of my lungs like a pebble. Can’t pull it apart.
Blood in yours?
Brownish. I need Kleenex all the time. It just comes up.
We’re at a box and a half of Kleenex a day. We’re down to our last box now.
I’m sick but you can’t tell I’m sick.
That’s Tim.
Aubrey teaches first grade. She will complete this semester and then resign. She experiences fainting spells and can no longer risk driving to work. She never knows when it will happen. She carries an inhaler with her at all times and has a nebulizer at home.
I have a job, kids, Aubrey says. I can’t drop everything and drive to St. Louis to argue with the VA.
Shanna nods. We had one appointment, she says, they were reading a book on how to give Tim a nerve test. We have to do a nerve test, they said. I said, You did one yesterday. I brought him in. He was being jolted by electricity. They didn’t know what they were doing.
I’m going to apply for unemployability, Aubrey says.
You can but they shot us down. Sores?
Look like zits, but they’re not zits. They are everywhere.
Yeah, Tim gets them too. White stuff pops out. Feel like rocks. Trouble hearing?
No, I used to get ringing.
That’s 10 percent disability automatically.
They denied me, Aubrey says.
Another report related to burn pits—this one from the government’s own watchdog agency, the Government Accountability Office, dated October 2010—states that, after a decade of war, the Department of Defense has been failing to adhere to its own policies regarding burn pit safety. The GAO’s summary concludes:
From the start of military operations in Afghanistan and Iraq, the US military and its contractors have burned solid waste in open burn pits on or near military bases. According to the Department of Defense (DOD), burn pit emissions can potentially harm human health …
Despite its reliance on burn pits, CENTCOM did not issue comprehensive burn pit guidance until 2009. Furthermore, to varying degrees, operators of burn pits at four bases GAO visited in Iraq were not complying with key elements of this guidance, such as restrictions on the burning of items, including plastic, that produce harmful emissions. DOD officials also said that, from the start of each conflict, operators routinely burned items that are now prohibited; The continued burning of prohibited items has resulted from a number of factors, including the constraints of combat operations, resource limitations, and contracts with burn pit operators that do not reflect current guidance.
I think of something Doctor Szema told me: fighting wars, the last thing the military worries about is trash disposal. But if it affects troops, they should worry about it.
I never tell Tim and LeRoy about my cough and the pressure on my chest. My complaints, whatever their origins, do not compare to theirs, and I feel more than a little ashamed worrying about it. I will visit my doctor every four months and try not to worry.
On my last day in Robstown, LeRoy and I drive to a supermarket to pick up a few things for Rosie. He mentions that she wants him to see another doctor in Denver, an abdominal specialist. The very idea wearies him. He is tired of doctors, tired of check-ups, tired of no one having an answer. This doctor, Rosie was told, thinks constrictive bronchitis is progressive. She got upset and LeRoy pulled her aside. Let’s don’t assume the worst, he told her. Let’s appreciate today.
On Sundays, LeRoy enjoys playing his guitar and singing at the church where his mother is pastor. The Spanish hymns lift him from his pain. Before he got sick, he could sing high notes like nobody’s business. No longer.
My drive the next morning takes me from Robstown through San Antonio, Austin, Dallas, and eventually to St. Louis, where I stop to see Tim and Shanna one more time.
In my absence, the VA has provided Tim with an electric wheelchair and an electric lift for their truck. Neither works. Tim is livid, swearing to stop dealing with the VA, stop dealing with doctors, stop dealing with all of it. He coughs, throws phlegm-filled Kleenex on the floor. Shanna steps into the garage, smokes a cigarette and weeps.
If I die, would you give up? Tim asks her when she comes back inside. His voice is soft. A sad expression on his face. The hurt and anger still there, too. Shanna looks at him, this man she married ten days after meeting him. The father of her children. The man she has loved for twenty-six years and who she thought might die in a war but who survived and came home.
No, she says finally. But I wouldn’t think it was fair.
[Both the Department of Defense and the US Department of Veterans Affairs declined to comment for this article.]















